Intelligent Automation for Healthcare RCM Workflows
Transform RCM processes into intelligent, automated workflows that drive faster reimbursement and sustained revenue growth
Trusted by over 2,000 of the world’s leading companies
Modernizing RCM with Intelligent Automation
Lower cost-to-collect through intelligent automation
AI-Powered Eligibility & Intake Automation
Intelligent Coding & Documentation Assist
Revenue Integrity & Compliance Monitoring
RCM Workflow Copilots for Operations Teams
Enterprise RCM Knowledge Intelligence
Enterprise RCM Data Integration & Modernization
Governed, Production-Grade Implementation
Clear oversight, auditability, and structured deployment ensure AI operates reliably within healthcare’s regulatory and compliance requirements.
Improved Denials prevention and first-pass yield
AI-enabled coding and claim management reduced denial rates by 18% and improved first-pass yield from 85% to 92% with $40M net revenue impact in a year for a health system. (HFMA, 2026)
Driving Cost-to-collect reductions
AI-enabled RCM could reduce the cost to collect by 30–60%, refocusing staff on high-value work rather than administrative tasks. (McKinsey & Company, 2026)
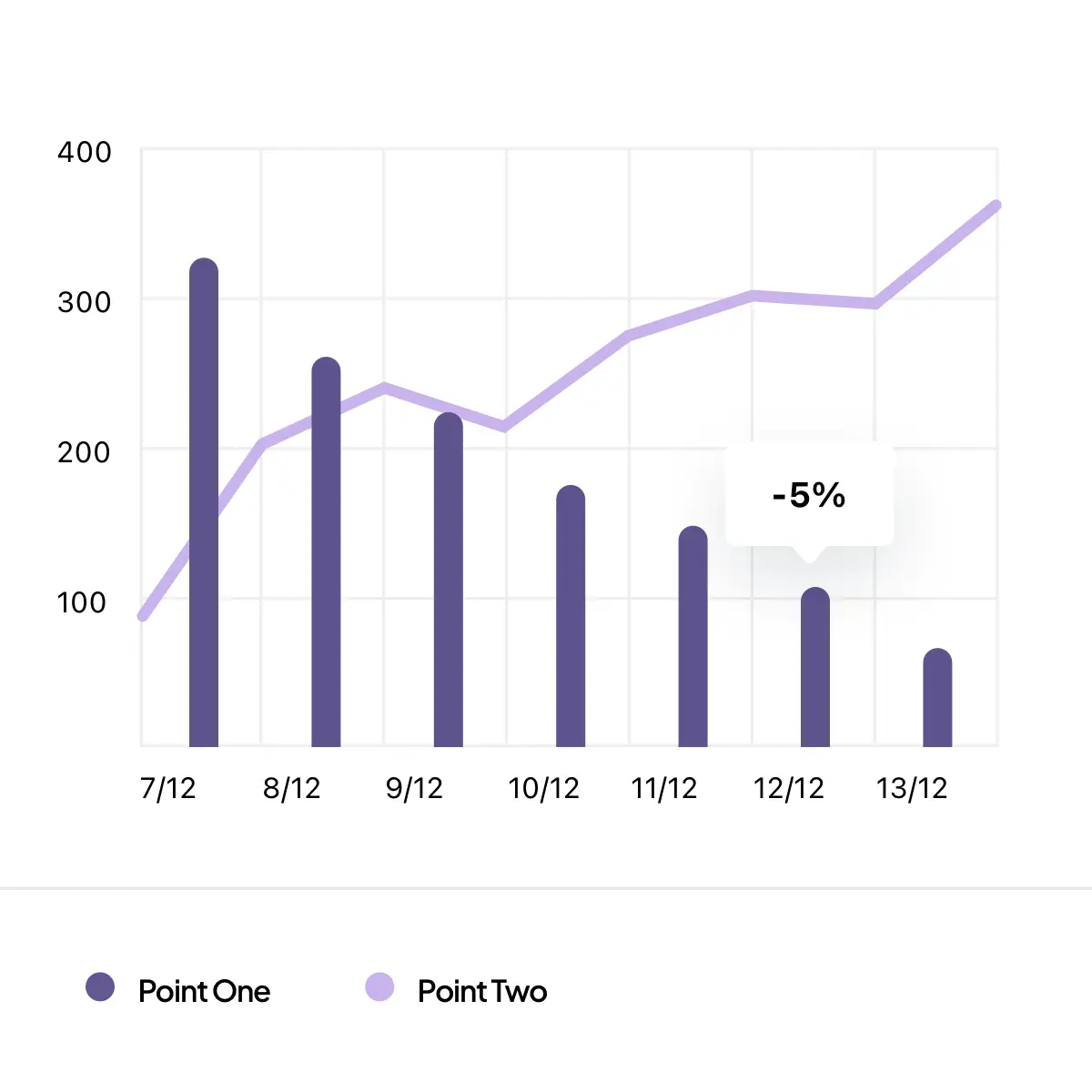
Adoption and organizational endorsement
46% of hospitals and health systems now use AI in RCM, and 82% of healthcare leaders consider AI integral to revenue cycle operations, showing broad industry confidence. (AHA, 2025)
Enhance Revenue Operations with AI-Driven RCM Solutions
Our AI-powered RCM solutions modernize workflows, strengthen revenue integrity, and optimize financial performance through automated coding, denial prevention, and seamless system integration across the healthcare revenue lifecycle.
Scalable RCM Transformation
Our solutions integrate AI, data, and workflows to drive measurable efficiency, improve accuracy, and accelerate reimbursement across complex healthcare environments.
Tonya M
“We Gained Accuracy, Speed, and Time Without Adding Staff.”
Adopting AI-powered coding has been one of the best decisions we’ve made. Our team is no longer buried in manual coding tasks or second-guessing payer requirements. The AI tool ensures greater accuracy, flags potential errors before claims go out, and keeps us compliant with evolving payer rules. The result? Fewer denials, faster reimbursement, and more time for my staff to focus on patient and practice needs instead of administrative backlogs. It truly feels like we’ve gained an extra layer of support and time without adding headcount.
Rated 4.9 of 5




